For decades, cancer treatment has relied on surgery, chemotherapy, and radiation. While effective, these approaches often come with significant side effects and limitations. In recent years, immunotherapy, especially CAR-T cell therapy, has transformed outcomes for certain cancers. But now, a breakthrough could push the field even further.
Scientists have developed a method to engineer cancer-fighting immune cells directly inside the patient’s body, potentially eliminating the need for complex laboratory procedures.
This innovation is being described as one of the most promising advancements in modern oncology.
Understanding the Basics: What Is CAR-T Cell Therapy?
CAR-T cell therapy (Chimeric Antigen Receptor T-cell therapy) is a personalised cancer treatment that modifies a patient’s immune system to target cancer cells.
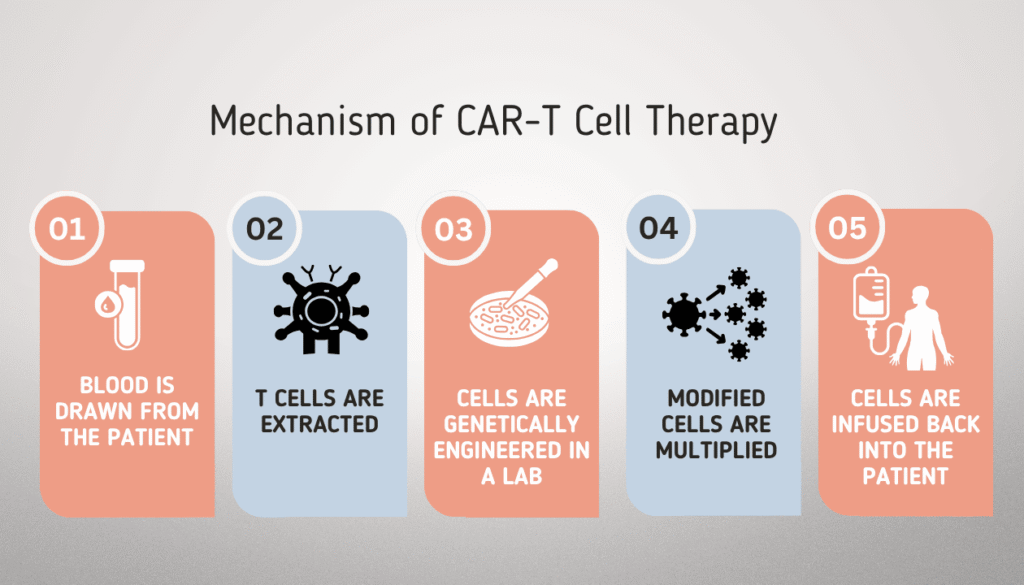
How Traditional CAR-T Therapy Works
5 easy Steps to Get Treated Abroad

Share Case Details

Get Expert Opinion and Hospital Quotes

Get Visa Invitation & Hotel Recommendations

Get Received At Airport and Start Your Treatment

Travel Back and Get Followups Through Us
- Blood is drawn from the patient
- T cells are extracted
- Cells are genetically engineered in a lab
- Modified cells are multiplied
- Cells are infused back into the patient
Once inside the body, these engineered T cells identify and destroy cancer cells.
Proven Success
CAR-T therapy has shown remarkable results in:
- Acute lymphoblastic leukemia (ALL)
- Diffuse large B-cell lymphoma (DLBCL)
- Multiple myeloma
In some cases, patients with no other options have achieved long-term remission.
The Major Limitations of Traditional CAR-T Therapy
Despite its success, CAR-T therapy faces critical challenges:
Extremely High Cost
Treatment can cost $400,000+, making it inaccessible for many patients globally.
Complex Manufacturing Process
- Requires specialised labs
- Takes 2–6 weeks
- Risk of delays or manufacturing failure
Limited Availability
Only a few advanced centers worldwide can offer this therapy.
Not Effective for All Cancers
- Strong success in blood cancers
- Limited effectiveness in solid tumours
Safety Concerns
- Cytokine release syndrome (CRS)
- Neurological side effects
These barriers highlight the need for a simpler, scalable alternative.
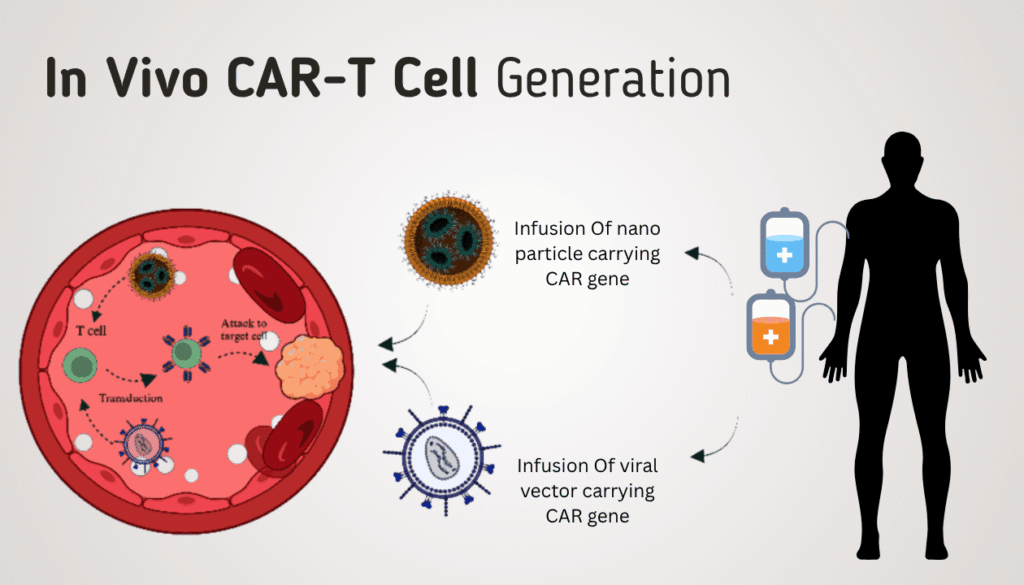
The Breakthrough: In Vivo CAR-T Cell Generation
Researchers from the University of California, San Francisco (UCSF), along with collaborating institutions, have developed a novel approach to generate CAR-T cells inside the body (in vivo).
Instead of extracting and modifying cells externally, this approach:
- Delivers genetic instructions into the bloodstream
- Targets T cells inside the body
- Reprograms them to attack cancer
This eliminates the need for lab-based cell engineering.
How Does This Technology Work?
The innovation relies on targeted gene delivery systems.
Step-by-Step Mechanism
- A specially designed vector carries genetic instructions
- The vector selectively targets T cells
- The CAR gene is inserted into the T cell DNA
- T cells become cancer-fighting CAR-T cells inside the body
- These cells multiply and attack tumours
Why This Is Revolutionary
- No cell extraction required
- No lab manufacturing
- Faster treatment delivery
- Potential for large-scale use
The Science Behind the Breakthrough
The study, published in Nature, demonstrates a highly precise gene-editing strategy.
Key Scientific Innovations
- Targeted DNA insertion at specific genomic locations
- Selective T-cell targeting, minimising off-target effects
- Use of advanced delivery systems (non-viral or engineered vectors)
- Stable and durable CAR expression
This level of precision is critical for safety and long-term effectiveness.
Study Results: What Did Researchers Find?
Preclinical studies (animal models) showed highly promising outcomes:
Blood Cancers
- Effective against leukemia
- Strong response in multiple myeloma
Solid Tumours
- Significant tumour reduction
- A major breakthrough since CAR-T struggles with solid cancers
Speed of Response
- Tumour elimination observed in weeks
Performance Comparison
- In vivo-generated CAR-T cells performed equally or better than lab-made cells
Why This Breakthrough Could Change Global Cancer Care?
This innovation could address several major challenges in cancer care, including:
- Drastically Lower Costs
Removing lab manufacturing could dramatically reduce treatment costs.
- Faster Treatment Access
Patients could receive therapy within days instead of weeks.
- Expanded Global Availability
Hospitals without advanced biotech labs could offer treatment.
Improved Patient Experience
- Less invasive
- Reduced waiting time
- Potentially fewer side effects
Scalability
This method could bring advanced immunotherapy to millions of patients worldwide.
What About Safety?
Safety remains a critical consideration.
Potential Risks
- Off-target gene editing
- Immune overactivation
- Long-term genetic effects
What Researchers Are Doing
- Improving targeting precision
- Conducting extensive preclinical testing
- Planning controlled human trials
Is This Treatment Available in India or Abroad?
Currently, this therapy is not yet available for patients.
Current Status
- Preclinical research stage
- Human clinical trials expected next
However, traditional CAR-T therapy is available in:
- India (limited centers)
- USA
- Germany
- Turkey
CancerRounds can help patients explore these options globally.
The Future of Cancer Treatment: What Comes Next?
This breakthrough signals a shift toward:
In Vivo Therapies
Treatments created inside the body rather than in labs.
Personalised Medicine at Scale
Tailored therapies without complex infrastructure.
Expansion to More Cancers
Including solid tumours like:
Combination Therapies
Pairing in vivo CAR-T with:
- Immunotherapy
- Targeted therapy
Expert Perspective
Many scientists believe this innovation could:
- Democratise advanced cancer care
- Reduce dependency on specialised labs
- Accelerate the adoption of gene-based therapies
If successful in humans, this could become one of the most important milestones in oncology.
Final Thoughts: A Hopeful Future for Cancer Patients
The ability to create cancer-fighting cells directly inside the body represents a paradigm shift in medicine.
While more research is needed, this innovation has the potential to:
- Make life-saving treatments accessible
- Reduce financial burden
- Improve survival rates worldwide
For patients and families navigating cancer, this breakthrough offers something invaluable: hope backed by science.
 Chat on WhatsApp
Chat on WhatsApp